Compression therapy uses controlled air pressure to support circulation, reduce swelling, and speed up recovery in muscles and tissues. When you wear compression garments or use pneumatic devices, they gently squeeze your limbs, helping blood flow back to the heart and lymphatic fluid move efficiently. This prevents blood pooling and fluid buildup, reducing soreness and inflammation. If you want to understand how these devices work and choose the right options, keep exploring further.
Key Takeaways
- Air pressure from compression devices applies controlled external force to limbs, enhancing circulation and reducing swelling.
- It promotes blood flow by squeezing tissues, preventing blood pooling, and aiding oxygen delivery to muscles.
- Compression stimulates lymphatic vessels, improving waste removal and reducing inflammation for faster recovery.
- Properly calibrated air pressure supports vein walls, easing blood return to the heart and preventing circulation issues.
- Wearable and pneumatic devices allow adjustable pressure, optimizing therapeutic benefits and comfort during recovery.
What Is Compression Therapy and How Does It Work?
Have you ever wondered how compression therapy helps improve circulation and reduce swelling? It works by applying controlled pressure to your limbs, promoting better blood flow and lymphatic drainage. The compression benefits include easing discomfort, preventing blood clots, and speeding up recovery. To maintain these benefits, device maintenance is essential; keeping your compression equipment clean and in good working order ensures peak performance and longevity. Most devices are designed for easy upkeep, so regular inspections and proper storage are simple steps you can take. When used correctly, compression therapy can be a powerful tool in managing swelling and enhancing circulation. Understanding how it works and caring for your device helps you get the most out of your treatment. Additionally, smart device maintenance can help monitor and optimize your therapy sessions for better results. Proper device upkeep not only ensures safety but also extends the lifespan of your equipment, making your therapy more effective over time. Regular cleaning and preventive checks are crucial for maintaining consistent therapy quality, especially given the importance of equipment longevity in healthcare devices. Moreover, paying attention to filtration systems and ensuring they are functioning correctly can significantly improve device performance and patient comfort.
How Does Air Pressure Improve Circulation?
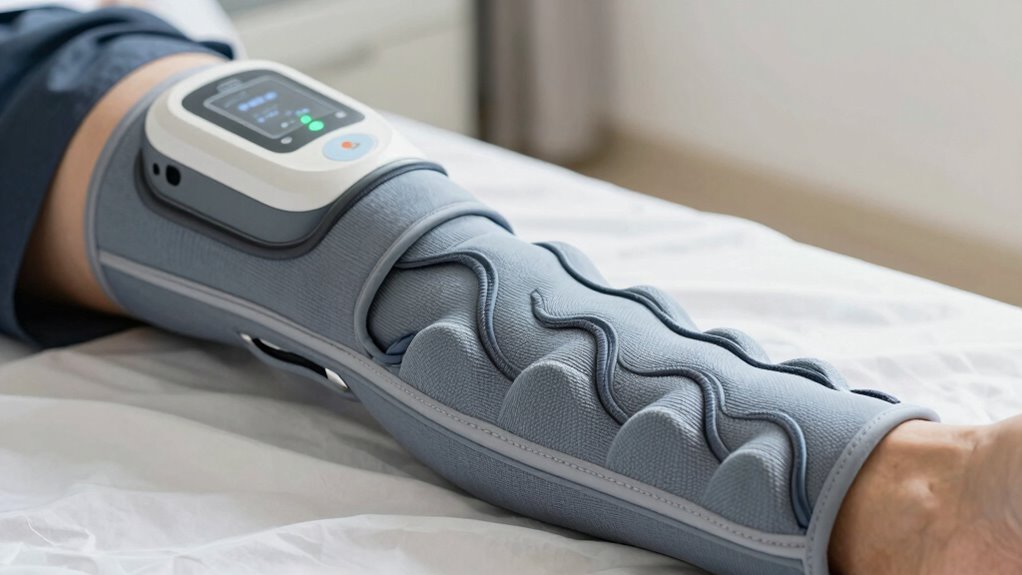
Air pressure from compression therapy helps boost your blood flow, making circulation smoother and more efficient. It also lowers the pressure in your veins, reducing swelling and discomfort. Additionally, it encourages lymphatic drainage, which helps your body eliminate waste and toxins more effectively. This process supports overall tissue health and promotes faster recovery. Circulatory system plays a key role in how compression therapy benefits your body. Interestingly, the influence of external pressure on blood flow has been studied in various contexts, highlighting how external forces can impact your vascular health. Moreover, understanding the impact of external forces on blood vessels can help tailor effective treatment approaches. External pressure applied with the right intensity can optimize vascular response, leading to improved recovery outcomes. Recognizing how pressure levels are managed is crucial for maximizing the benefits of compression therapy.
Enhances Blood Flow
When air pressure is applied through compression therapy, it actively encourages better blood flow by gently squeezing the underlying tissues and vessels. This compression helps maintain ideal blood circulation, preventing stagnation and reducing the risk of blood pooling in the extremities. As a result, oxygen-rich blood reaches your muscles more effectively, supporting faster recovery and reducing fatigue. Improved blood flow also promotes the removal of metabolic waste products, which can cause soreness and swelling. Additionally, the calibration process of compression devices ensures consistent pressure application, optimizing circulation and healing. By enhancing circulation, compression therapy supports overall vascular health, keeping your blood vessels flexible and resilient. This process not only aids in recovery but also contributes to long-term circulatory efficiency, helping you stay active and healthy. Proper application of compression therapy ensures consistent pressure that optimizes circulation and enhances healing. Additionally, sustained improved circulation can help prevent future vascular issues, promoting overall circulatory health. Regular use of compression therapy can also help improve vascular resilience, making your circulatory system better equipped to handle daily stresses. Furthermore, maintaining proper pressure levels is crucial for achieving the best therapeutic outcomes and avoiding potential discomfort.
Reduces Venous Pressure
Applying controlled air pressure through compression therapy directly reduces venous pressure in your legs and arms. By compressing your blood vessels, it helps prevent blood pooling, which can occur when blood struggles to return to the heart. Lower venous pressure means less strain on your veins, reducing the risk of swelling and discomfort. When blood pools, your veins can become distended, increasing the likelihood of varicose veins and other circulation issues. Compression garments apply consistent pressure that supports the vein walls, making it easier for blood to flow upward. This not only alleviates venous pressure but also encourages healthier circulation, helping your body efficiently return blood to your heart. Additionally, using specialized compression devices can optimize pressure levels for different body areas, further enhancing circulation benefits. Overall, managing venous pressure with compression therapy promotes better circulation and reduces the risk of circulatory problems.
Promotes Lymphatic Drainage
How does compression therapy enhance lymphatic drainage? It stimulates lymphatic function by applying controlled air pressure, which encourages fluid movement through your lymphatic vessels. This increased pressure helps to improve fluid clearance from tissues, reducing swelling and preventing fluid buildup. As compression gently compresses your limbs, it creates a pressure gradient that directs lymph toward your lymph nodes for processing and removal. This not only accelerates waste removal but also boosts immune function. By promoting efficient lymphatic flow, compression therapy supports your body’s natural detoxification process, reduces discomfort from edema, and helps you recover faster. Additionally, proper air pressure regulation ensures the therapy remains safe and effective. Understanding the flow dynamics of lymphatic circulation can help optimize treatment outcomes. Moreover, integrating consistent application of compression techniques can enhance overall effectiveness and ensure sustained benefits. Proper technique adherence is essential for maximizing the benefits of compression therapy and preventing potential complications. Furthermore, maintaining an awareness of pressure levels can help tailor therapy to individual needs, enhancing results and safety. Overall, the improved circulation from compression ensures your lymphatic system works at its best, maintaining a healthy balance of fluids and supporting overall healing.
What Are the Types of Compression Devices for Therapy?

There are different types of compression devices you can use for therapy, including manual and mechanical options. Some devices are wearable, like sleeves and wraps, while others are stationary machines. Understanding these options helps you choose the best fit for your needs and lifestyle. Selecting the right equipment ensures you maximize safety and effectiveness during recovery. Proper device maintenance is also essential to ensure consistent performance and longevity of your compression therapy tools. Knowing the appropriate application techniques can further improve treatment outcomes and prevent potential issues. Additionally, familiarizing yourself with device features can help optimize your therapy sessions and adapt to your specific recovery goals.
Types of Compression Devices
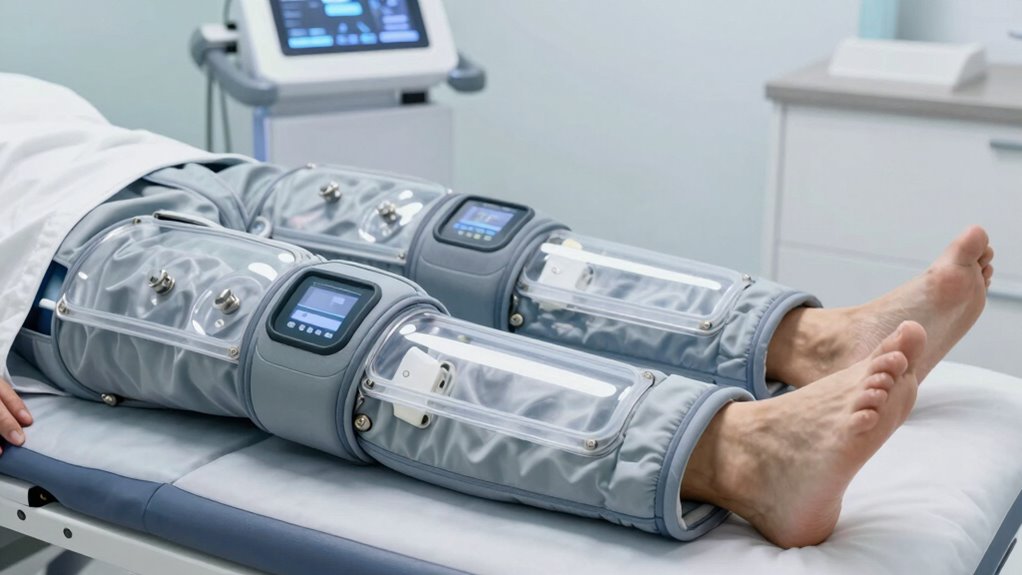
Various types of compression devices are designed to meet different therapeutic needs, offering flexibility and customization for patients. Compression garments are one of the most common options; they are tight-fitting sleeves, stockings, or wraps made from elastic materials that apply consistent pressure to your limbs. These are often used for ongoing management of conditions like edema or varicose veins. Pneumatic devices, on the other hand, involve inflatable cuffs or sleeves connected to a pump, which intermittently inflate and deflate to provide controlled compression. This type is especially useful for more targeted or intensive therapy sessions. Both compression garments and pneumatic devices allow you to tailor the pressure and coverage, ensuring you receive effective treatment suited to your specific recovery or health needs.
Manual vs. Mechanical Devices
When it comes to compression therapy, you can choose between manual and mechanical devices, each offering distinct advantages. Manual devices rely on your hand or a caregiver’s skill to apply pressure, making them suitable for customized compression techniques and flexible therapy protocols. They are portable and cost-effective but require consistent effort for effective results. Mechanical devices, on the other hand, use pumps or automated systems to deliver precise, controlled air pressure. These are ideal for maintaining consistent therapy protocols, especially during extended sessions or for users with limited mobility. Mechanical options often feature adjustable settings for different levels of compression, ensuring ideal support. Your choice depends on your specific needs, comfort, and the level of consistency required for effective recovery.
Wearable and Stationary Options
Compression therapy devices come in both wearable and stationary forms, each designed to suit different treatment needs and lifestyles. Wearable devices, such as compression garments, are flexible and easy to use throughout the day or night. They include sleeves, stockings, and wraps that provide consistent pressure directly to target areas. These garments are popular for ongoing management of conditions like swelling or varicose veins. Stationary options, on the other hand, involve devices like pneumatic compression pumps. You typically use these in a clinical setting or at home, where the device inflates cuffs around your limbs to apply controlled pressure. Both types are effective, but your choice depends on your mobility, comfort preferences, and treatment goals. Knowing your options helps you select the best device for your recovery process.
How Does Compression Help Reduce Swelling and Edema?
How exactly does compression help reduce swelling and edema? The compression benefits work by applying steady pressure to your limbs or affected areas, which helps improve blood flow and lymphatic drainage. This pressure prevents fluid from accumulating in tissues, effectively reducing edema. When your tissues are compressed, it encourages the excess fluid to move back into your bloodstream for removal. By supporting the vessels and limiting the space where fluid can collect, compression therapy minimizes swelling and speeds up recovery. It’s especially helpful after injury or surgery, where swelling can hinder healing. Overall, compression offers a targeted way to manage edema, providing comfort and aiding your body’s natural processes to restore balance and reduce inflammation.
How Can Compression Speed Up Muscle Recovery?

When you wear compression gear, it boosts your blood flow, delivering oxygen and nutrients to your muscles faster. This process helps reduce swelling and inflammation, speeding up recovery. By improving circulation, compression allows your muscles to heal more efficiently after workouts or injuries.
Enhances Blood Circulation
By applying consistent pressure to your limbs, compression therapy actively promotes better blood flow, which is essential for muscle recovery. This circulation improvement delivers oxygen and nutrients more efficiently to tired muscles, speeding up healing. Imagine your blood vessels as a network of rivers: compression gently narrows the channels, encouraging blood to flow upward and outward. This process enhances the overall flow, reduces stagnation, and boosts recovery. Here’s a visual to help you picture circulation benefits:
| Vessel Type | Effect of Compression | Result |
|---|---|---|
| Arteries | Narrow slightly | Faster oxygen delivery |
| Capillaries | Increased flow | Improved nutrient exchange |
| Veins | Enhanced return | Reduced muscle fatigue |
| Lymphatics | Stimulated flow | Less fluid buildup |
Reduces Swelling and Inflammation
Compression therapy effectively reduces swelling and inflammation after muscle exertion by applying steady pressure that encourages excess fluid to move out of tissues. This is one of the key compression benefits, as it helps decrease puffiness and discomfort. When you wear compression garments or use air pressure devices, they enhance lymphatic drainage and improve fluid circulation around injured muscles. As a result, swelling reduction occurs more quickly, reducing pain and stiffness. By minimizing inflammation, compression supports faster recovery and enables you to return to activity sooner. The consistent pressure prevents fluid buildup, keeps blood flowing, and promotes tissue healing. Overall, compression therapy plays a essential role in managing swelling and inflammation post-exercise, making your recovery more efficient and comfortable.
Is Compression Therapy Right for You?

Deciding if compression therapy is right for you involves considering your specific health needs and lifestyle. Not everyone benefits equally, so understanding your suitability is key. Compression benefits include improved circulation, reduced swelling, and faster recovery, but patient suitability varies. Ask yourself: Do you have circulation issues, varicose veins, or recent surgery? Consulting your healthcare provider will help determine if compression therapy fits your goals. Here’s a quick overview:
| Considerations | Suitability Questions |
|---|---|
| Circulation health | Do you experience swelling or heaviness? |
| Medical conditions | Are you recovering from surgery? |
| Lifestyle factors | Are you active or have mobility issues? |
This will guide you toward making an informed choice.
How to Choose the Best Compression Garments and Devices

Choosing the right compression garments and devices can markedly enhance your therapy results, but with so many options available, it’s vital to know what to look for. Start by considering fabric materials—look for breathable, moisture-wicking fabrics like nylon or spandex blends that provide comfort and durability. Proper garment sizing is essential; an ill-fitting compression item won’t deliver the right pressure and may cause discomfort or restrict circulation. Measure your limbs accurately and consult sizing charts from manufacturers to guarantee a snug, yet comfortable fit. Additionally, think about the type of device or garment that suits your needs—whether it’s sleeves, stockings, or wraps. Selecting high-quality, well-fitting compression gear tailored to your body ensures maximum support and recovery.
Myths and Facts About Compression Therapy

Many people believe that compression therapy is a quick fix or only needed for severe conditions. This is a common compression myth. In reality, therapy facts show that consistent use improves circulation and aids recovery, but it’s not a cure-all. Some think compression garments are uncomfortable or restrict movement; however, proper fit and gradual adjustment make them comfortable. Here’s a quick comparison:
| Compression Myths | Therapy Facts | Clarifications |
|---|---|---|
| It’s only for serious injuries | It supports minor issues too | Suitable for everyday use |
| It’s uncomfortable | When fitted properly, it’s comfortable | Proper sizing is key |
| It’s a quick fix | Requires consistent use for best results | Not a one-time solution |
| It’s only for athletes | Benefits everyone with circulation issues | Not just for sports |
| It replaces medical treatment | It complements medical care | Consult healthcare providers |
Safety Tips and When to See a Healthcare Provider

While compression therapy offers many benefits, it’s vital to follow safety guidelines to prevent potential complications. Always consult a healthcare professional before starting therapy to guarantee proper fit and pressure levels. If you experience increased pain, numbness, or skin discoloration, stop using the compression device and seek medical advice promptly. Proper compression safety minimizes risks like circulation issues or nerve damage. Be cautious if you have underlying conditions such as heart problems or diabetes, and always get a therapy consultation if unsure. Regularly check your skin for redness or irritation, and avoid overly tight garments. Remember, compression therapy isn’t one-size-fits-all; professional guidance helps you use it safely and effectively. Your healthcare provider can tailor recommendations to suit your specific needs.
Future Trends in Compression Therapy Technology
Advances in materials science and wearable technology are driving exciting innovations in compression therapy. You can expect devices that are more comfortable, effective, and tailored to your needs through smart technology and advanced materials. Future trends include smart compression garments that adjust pressure automatically based on your activity or recovery stage. These garments will use sensors to monitor circulation, providing real-time feedback. Here’s a glimpse of what’s coming:
| Feature | Benefit | Technology Used |
|---|---|---|
| Adaptive Pressure | Customizes compression levels instantly | Smart sensors and AI |
| Lightweight Fabrics | Increased comfort and mobility | Advanced materials |
| Data Integration | Tracks progress digitally | Wearable tech, apps |
| Energy Efficiency | Longer battery life, eco-friendly | Innovative power sources |
These innovations aim to optimize recovery, making compression therapy more effective and user-friendly.
Frequently Asked Questions
Can Compression Therapy Be Used During Physical Activity?
Yes, you can use compression therapy during physical activity to boost sports performance and aid injury prevention. Wearing compression garments helps improve circulation, reduce muscle fatigue, and provide support, which can enhance your endurance and recovery. Many athletes incorporate compression gear into their routines, finding it beneficial during training and competitions. Just ensure you choose the right level of compression and fit for comfort and ideal results.
How Long Should Each Compression Session Last?
You might think longer is better, but for compression therapy, shorter sessions often do the trick. Typically, you should aim for about 20 to 30 minutes per session, focusing on the most suitable timing for your recovery needs. Overdoing it can cause discomfort or even harm, so listen to your body. Keep sessions consistent, and you’ll see benefits without risking unnecessary strain or irritation.
Are There Any Side Effects of Using Compression Devices?
Yes, using compression devices can cause side effects like discomfort, skin irritation, or potential allergies. To minimize these risks, make certain the device compatibility with your skin and check for any allergies to materials used. Always follow the recommended settings and duration, and consult a healthcare professional if you experience persistent pain or unusual reactions. Proper fit and skin care are essential for safe and effective compression therapy.
Is Compression Therapy Effective for Chronic Conditions?
Like a steady anchor in turbulent seas, compression therapy offers reliable support for your chronic condition management. It’s effective as part of long-term therapy, helping improve circulation and reduce swelling. While it may not be a cure-all, consistent use can enhance your quality of life. You’ll find it’s a valuable tool in maintaining stability, especially when combined with other treatments, making your journey toward better health more manageable.
Can Children Safely Use Compression Therapy?
You should consult a healthcare professional before using compression therapy on children, as pediatric safety is key. While some devices are designed for child suitability, not all are appropriate for kids. They need proper fitting and supervision to prevent discomfort or injury. Always seek expert advice to guarantee the therapy’s safe and effective for your child’s specific condition, and never use adult equipment on children without professional guidance.
Conclusion
Think of compression therapy as a gentle orchestra conductor, guiding your body’s natural rhythms to harmony. By improving circulation and reducing swelling, it helps your recovery play out smoothly. When you choose the right devices and follow safety tips, you’re tuning your body’s performance for peak results. Embrace these therapies as a trusted partner in your health journey, turning the chaos of injury or fatigue into a symphony of healing.